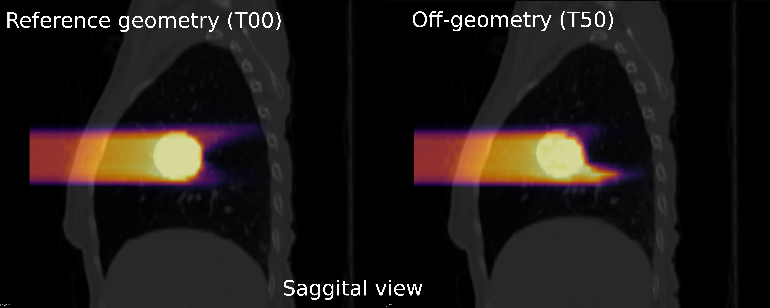
Terapija

Glavni cilj področja je razvoj bolniku prilagojenega zdravljenja z uporabo izboljšanih modelov tkiv in tumorjev v onkologiji (bolniku prilagojena radioterapija oz. druga terapija napredovanih rakov) ter nevrologiji (bolniku prilagojena obravnava pri nevrokognitivnih možganskih motnjah).